Perth's Leading Specialist in the Treatment of Varicose Veins
Dr Luke Matar | MBBS, FRANZCR, FACP
Why Skin Changes In Your Legs Are Important
Skin changes in your legs such as discolouration, itch, and dryness can indicate the presence of conditions such as venous eczema or ulcers.
What Should I Be Looking For?
 Changes on the skin surface can indicate an underlying issue in the deeper veins below. It’s important to pay attention to changes like these as if left untreated, symptoms can progress and worsen.
Changes on the skin surface can indicate an underlying issue in the deeper veins below. It’s important to pay attention to changes like these as if left untreated, symptoms can progress and worsen.
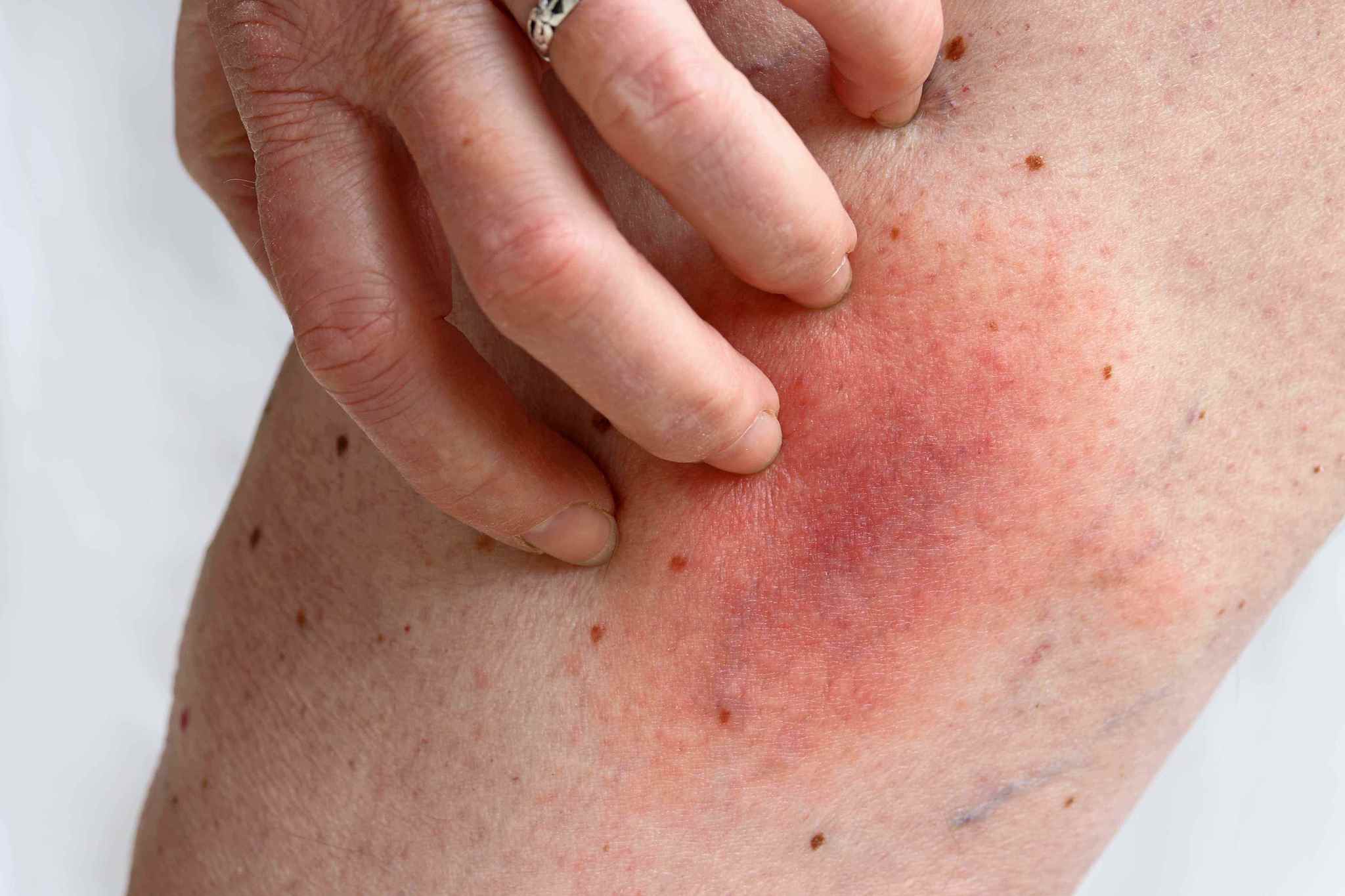
Look for changes in the condition of the skin, such as dryness or skin peeling. Itch or rash on your legs may indicate venous eczema is developing. Tenderness, warmth, redness, or swelling are all indications that you should take seriously and have a medical professional investigate at your earliest convenience.
The development of red, brown or “rust-like” patches (hemosiderin staining, or venous eczema), are an early warning sign that an ulceration may occur. Eventually, white patches (atrophe blanche) may form, heralding the breakdown of the skin and leading to ulcer development.
Venous Eczema
Venous eczema, also known as varicose eczema or stasis dermatitis, is an inflammatory condition of the skin seen in association with venous reflux. The skin becomes itchy, red and swollen, dry and flaky or scaly and crusty. It is usually found around the ankles or lower legs and frequently misdiagnosed by general practitioners as cellulitis or simple eczema.
Venous reflux occurs when the valves in the veins fail and blood travels toward the feet instead of the heart. This increases the pressure in the veins, which can cause fluid to leak into the surrounding tissues. It is thought that varicose eczema may develop as a result of the immune system reacting to this fluid.
Varicose eczema is more common in people with varicose veins, but not all patients with venous reflux and venous eczema will have visible varicose veins, as the varicose veins may be “hidden”. Prevention is therefore the best “cure” to stop this condition from progressing and worsening over time. Early intervention is ideal, so if you recognise these symptoms, contact us today.
Venous Ulcers
Venous leg ulcers are the most severe consequence of untreated venous reflux, but fortunately, they are often preventable and treatable. It is estimated that 1% of the general population and 5% of patients with varicose veins will develop a chronic venous ulcer during their life.
Once established, they can lead to a significant decrease in quality of life and patients may experience social and economic decline. Like all things health related, prevention and early action is key.
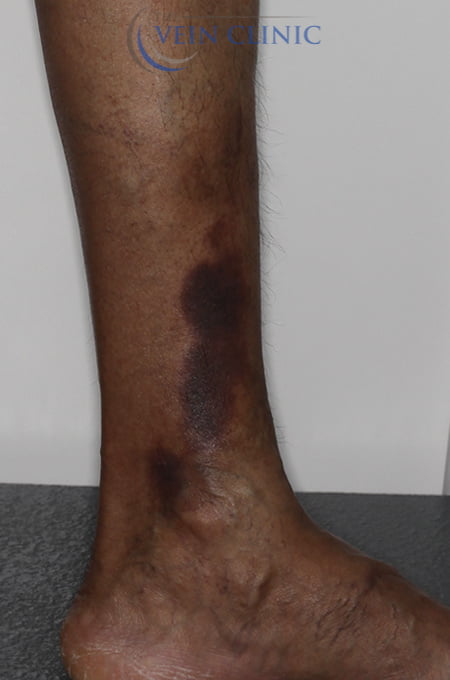
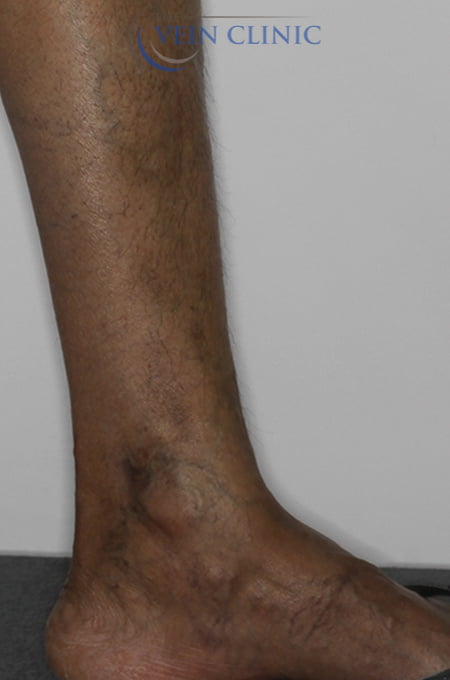
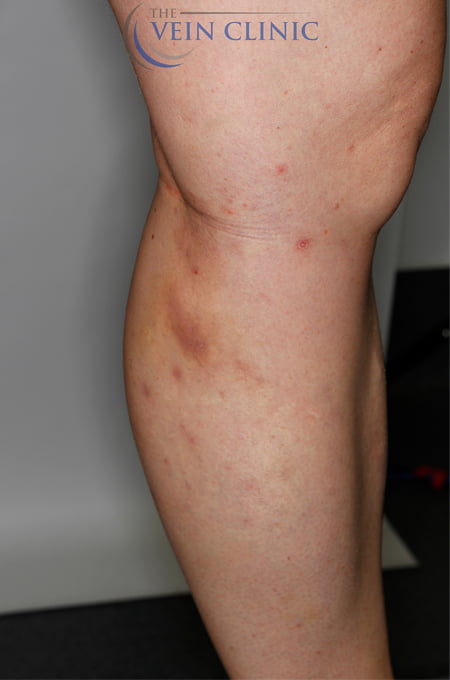
Skin Changes Treatment Before & Afters
Treatment Method
Endovenous laser ablation (EVLA) and ultrasound-guided foam sclerotherapy (UGFS)
Read MoreOur Approach to Vein Treatment
Stage 1
Treatment of large malfunctioning veins (trunk)

Endovenous Laser Treatment (EVLA) to great, small, and/or anterior accessory saphenous veins. 60 minutes
Stage 2
Treatment of large varicose veins (branches)

Phlebectomy removal of larger bulging varicose veins 90-120 minutescombined with

Ultrasound-Guided Foam Sclerotherapy (UGFS) on smaller veins. 30 minutes
Stage 2
Treatment of small varicose veins (branches) if required

Extra sessions of UGFS to close smaller veins if identified as required at post-treatment follow-up scan 30 minutes
You may not require this stage.
Stage 3
Optional treatment surface veins (leaves)

Usually done by Microsclerotherapy 30 minutes
Most patients require multiple treatment sessions to remove spider veins.
Stage 4

Follow up and maintenance to ensure best results
Our Minimally Invasive
Treatments
Experiencing Other Symptoms?
Frequently Asked Questions
Why do I have varicose veins?
Most varicose vein issues are hereditary. If you have one parent with varicose veins your risk of having them is around 65%. If both parents are affected the risk rises to approximately 90%. Another main risk factor for women is pregnancy, with the risk increasing with each additional pregnancy. Standing occupations such as hairdressers, nurses, and chefs also have a high risk of varicose veins as gravity puts pressure on the veins and weakens them.
How do I prevent varicose veins?
Once varicose veins are present, they will not resolve of their own accord. Measures to reduce the rate of progression include maintaining a normal healthy weight and going for regular walks of 20-30 minutes per day. Reducing the length of time spent on the feet in a stationary position may help and alternating between standing and sitting positions during the day will also reduce the pressure on the veins.
What will happen if I don’t treat these veins?
Generally, without treatment, varicose veins will get progressively worse over time. Symptoms may occur such as heaviness, ache, pain, and tiredness in the legs towards the end of the day. Further progression may result in leg swelling, itch, skin discolouration, and eventual skin ulceration. Blood clots related to superficial venous thrombosis may also occur in severe cases and can lead to the more serious condition of Deep Vein Thrombosis.
What treatment options exist?
Outdated, old-fashioned options such as surgical stripping are rapidly becoming obsolete due to poor long-term success, with recurrence rates of up to 50%. Modern treatment options include endovenous laser ablation, sclerotherapy injections, and ultrasound-guided ambulatory phlebectomy. In many cases a combination of different treatments will give the best long-term results.
Will the veins come back after treatment?
Many people are concerned that the treatment will be of limited value because the veins will just come back. This was certainly the case in the days of surgical stripping with a 50% recurrence rate at 5 years; however, using the latest minimally invasive techniques, we can reduce the risk of recurrent varicose veins to the baseline risk of approximately 3% per year.
What is the downtime following treatment?
This depends on the type of procedure performed and the severity of the veins being treated. Modern treatment with laser can involve no time off work and approximately two weeks off heavy gym work and four weeks off international travel.
Read More on Our Blog

5 Ways to Prepare for Your Vein Procedures
1. Get to know and love your stockings! We strongly recommend you buy your compression stockings well ahead of your […]
Read More
Don’t Be Fooled By Winter!
Cold weather constricts the veins and can make you feel “less symptomatic” – ie. the bothersome ache, pain, itch, heaviness, or tiredness in your legs could be less of an issue, or perhaps go away entirely.
Read More
Do I Need Varicose Vein Treatment?
Suffering from varicose veins? For too long patients have been told that treatment for varicose veins is “cosmetic only” and […]
Read MoreGet In Touch
Please send us an email and we’ll be in contact very soon or alternatively, call us on (08) 9200 3450.
If you are unsure of what vein condition you may have, assess your legs with our online tool.
If you are looking for cosmetic spider vein treatment only, please click here.