Perth's Leading Specialist in the Treatment of Varicose Veins
Dr Luke Matar | MBBS, FRANZCR, FACP
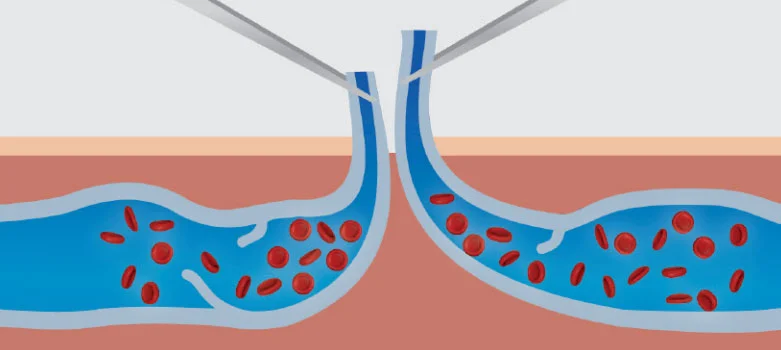
What is Ambulatory Phlebectomy?
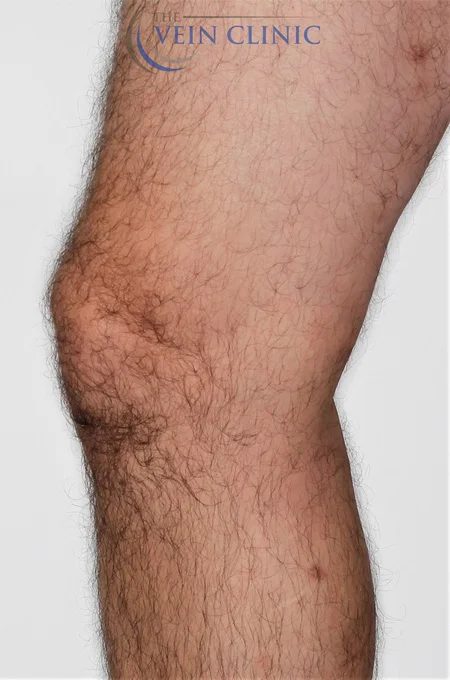
Ambulatory phlebectomy is a minimally invasive surgical technique used to remove bulging surface branch vessel varicose veins under local anaesthetic. Ambulatory phlebectomy usually provides the best cosmetic outcome and fastest relief from large bulging surface veins that may be difficult to treat with foam sclerotherapy alone.
Ultrasound-guided ambulatory phlebectomy is performed on a walk-in walk-out basis at our custom-built treatment clinic and you can return to your normal activities immediately, with only a two-week break from strenuous exercise.
This procedure combines the best of all technologies and even if it may sound a bit daunting to patients at first, it is usually very well tolerated. It allows for the most effective treatment of varicose veins, with the lowest chance of additional follow-up requirements.
Why Choose
Ambulatory Phlebectomy For Varicose Veins

Most Effective Treatment For Varicose Veins
Ambulatory phlebectomy is especially effective for veins too large to treat with foam sclerotherapy alone. Combined with endovenous laser ablation, this procedure gives great aesthetic results by removing the veins bulging above the surface of the skin.

Increased Accuracy Under Ultrasound Guidance
Dr Luke Matar has pioneered the highly advanced method of performing phlebectomy under ultrasound guidance. This results in increased accuracy of placement, resulting in fewer incisions and therefore quicker recovery.

Minimally
Invasive
The size of the incisions required are so small that stitches are usually not needed. This means that you can heal faster, allowing you to return to daily activities almost immediately.
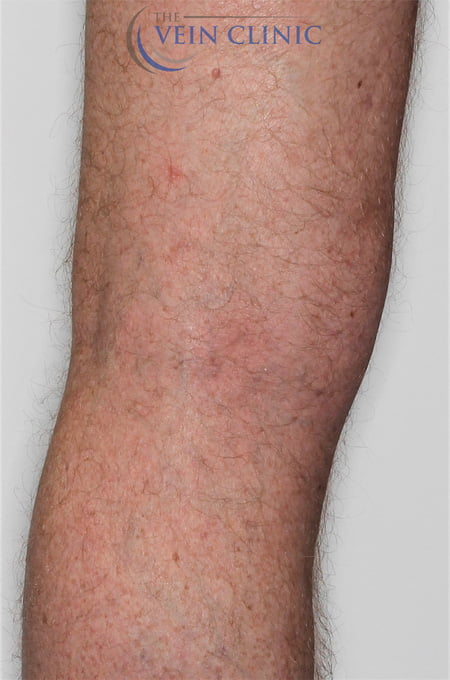
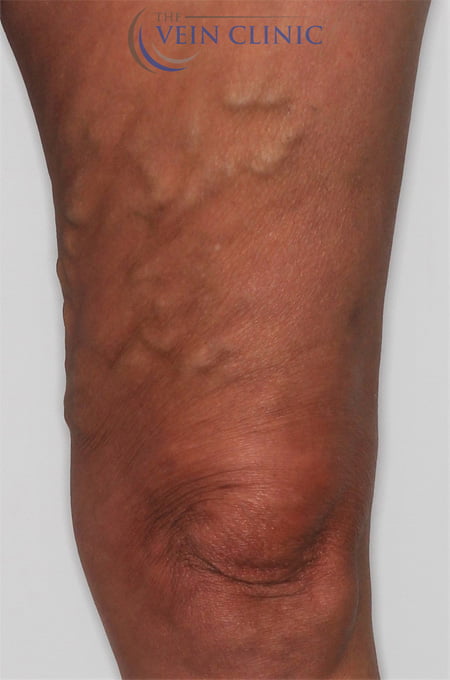
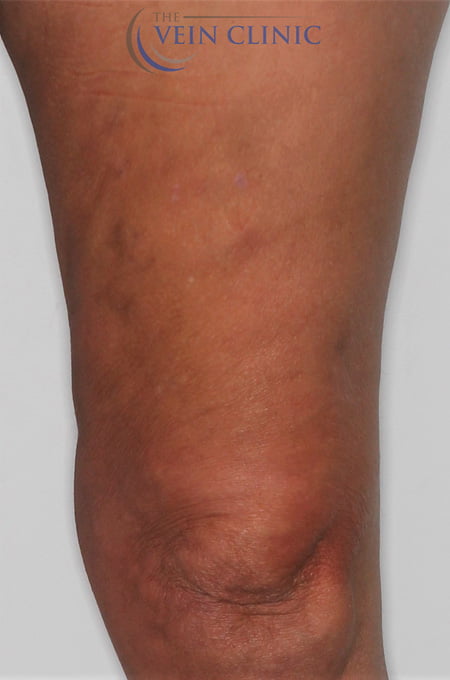
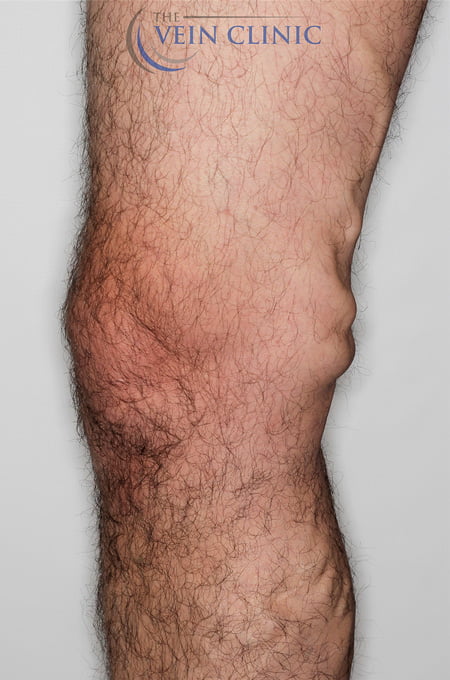
Ambulatory Phlebectomy
Before and Afters
How Does Ambulatory Phlebectomy Treatment Work
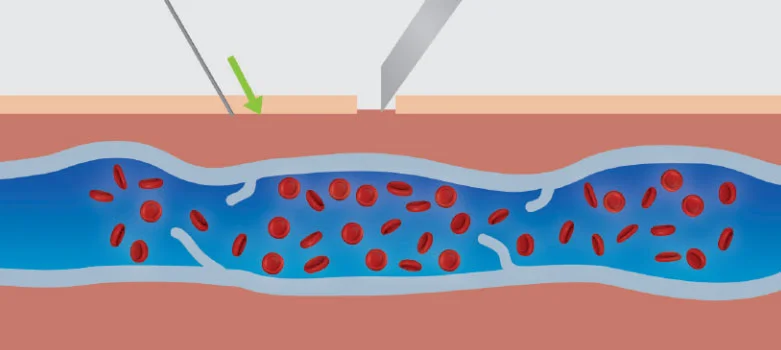
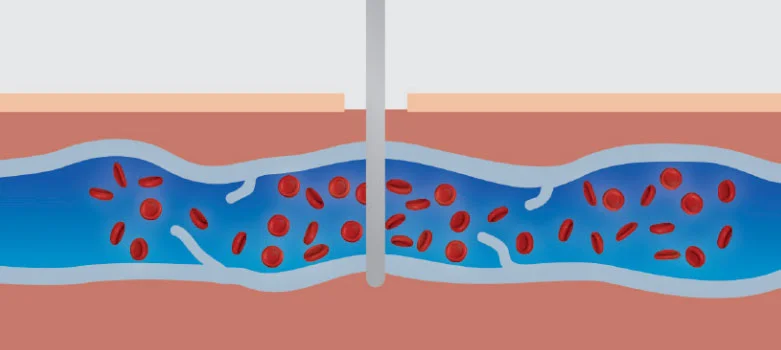
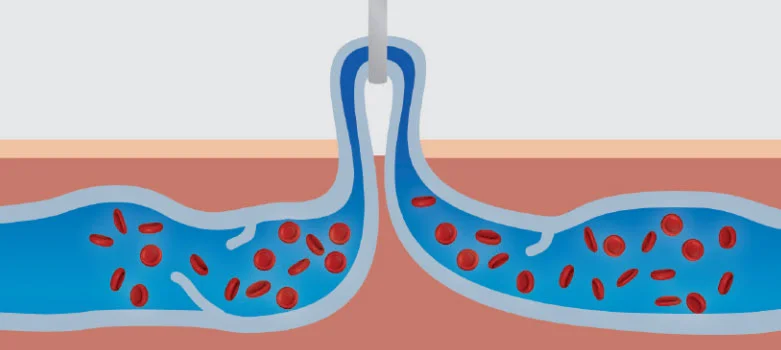
Ambulatory phlebectomy involves the physical removal of the varicose veins through multiple small incisions in the skin, directly overlying the vein. Veins are very collapsible and even large veins can be removed through the tiny incisions used in this technique.
Read MoreThe Procedure
What to Expect During & After Your Treatment
Prior to your treatment, you will first see our sonographer, who will carefully mark out the area to be treated using ultrasound. You will be given the opportunity to listen to your favourite music, read a book or simply chat with our friendly nurse whilst Dr Matar does his magic.
If you’re feeling anxious or nervous about the procedure, or if you have a low pain tolerance, please let us know ahead of time and we can arrange for our nurse to give you a pre-med mix of painkillers and a light sedative to relax you prior to the treatment.
The ambulatory phlebectomy procedure takes approximately 2 hours.
Ambulatory Phlebectomy Aftercare
After the procedure is complete we will apply a pressure foam bandage to tightly compress the veins, with compression stockings applied over this thick packaging. This can feel somewhat uncomfortable but is necessary to protect the leg and ensure proper recovery. This foam bandaging is to be removed after 4 days with the compression stockings to remain for a further 10 days.
Two weeks after your treatment you will return for a follow-up ultrasound scan so that we can remove your compression stocking and check on the incision wounds to see how your recovery is progressing. This scan is important to exclude the minimal risk of deep vein thrombosis and is a necessary step of your post-treatment aftercare plan.
Recovery Post Treatment
Most patients will heal quickly and wounds will be clean, closed and fully sealed after 2 weeks. Delayed healing is more common in the following situations:
- Patients that have had prior stripping/vein surgery
- Those with extremely large veins
- Smokers
- Diabetics
- Elderly
- Obese/overweight
- Immune compromised
- Poor nutrition
- Poor compliance with post op instruction
How to Find the Best Ambulatory Phlebectomy in Perth
What Makes the Vein Clinic Different?
Just because the treatment offered at a vein clinic is called ambulatory phlebectomy, doesn’t mean you will receive equal treatment across all clinics.
The Vein Clinic differs from its competitors not only in our level of expertise and experience but in every detail of how we operate and perform our world-class treatments.
Dr Matar has developed his own method of performing phlebectomy under precise ultrasound guidance. This extends the treatment length to 2-2.5 hours instead of 20-30 minutes, giving much better results due to the care and thoroughness Dr Matar applies. This means that veins are much less likely to recur as they were properly and carefully removed at the initial treatment, avoiding further re-treatments.
These differences alongside our expertise, experience, and passion, means you won’t find a higher quality treatment elsewhere.
Do I Need Ambulatory Phlebectomy For Varicose Veins?
You could benefit from ambulatory phlebectomy if you experience any of the following vein problems.
Other Minimally Invasive
Varicose Veins Treatments
Frequently Asked Questions
What is Ultrasound-Guided Foam Phlebectomy?
Phlebectomy is a method of treating larger branch vessels by removing them via incision. Dr Luke Matar has refined and improved this process by adding the use of ultrasound guidance to place each incision with extreme precision. He also uses foam sclerotherapy to treat veins that are too small to physically remove. These innovations create the method of ambulatory phlebectomy that we at The Vein Clinic refer to as Ultrasound-Guided Foam Phlebectomy.
What are the benefits?
This treatment results in a more complete vein removal over traditional surgery, speeding the recovery process, and optimising cosmetic results. The incisions are so small they usually do not require sutures, making the healing and recovery process even more efficient.
Is it painful?
UGFP is performed under ultrasound-guided nerve block and dilute local anaesthetic, meaning you usually won't feel any pain during the procedure other than the local needles used to numb your leg. You can elect to have this procedure performed under IV sedation if you prefer – ask our clinical team for more information.
How long does the procedure take?
This depends on the extent of veins to be removed and other patient factors and will usually be between 2-2.5 hours. If there are many veins or multiple areas to treat, Dr Matar may split the treatment up into 2 sessions of 2 hours each.
What are the side effects?
Whenever an incision is made in the skin there is a risk of bleeding, bruising, and infection. These risks are easily managed and controlled. Bleeding is usually easily controlled with bandages and (if needed) sutures and is rarely an issue unless you have a bleeding disorder or do not stop blood thinners prior to treatment.
Some bruising is to be expected and usually resolves over 2-6 weeks. Hirudoid cream from the chemist and Dermaka Cream (that we supply) will often reduce the bruising significantly.
Rarely inflammation or skin infection can occur at the incision site. A precautionary antibiotic before the procedure is usually given to reduce the chances of this occurring and the procedure is performed under sterile conditions like those in a formal operating theatre.
What is the recovery like?
You will have a tight compression bandaging applied after the procedure which is to be worn for 3-4 days. This protects the leg from accidental bumping and allows for protected healing. After 3-4 days, the bandaging is fully removed and regular compression via stockings continues for a further 10 days. You should be able to resume daily activities within 24 hours of the procedure. Strenuous activity should be avoided for 2 weeks.
Get In Touch
Please send us an email and we’ll be in contact very soon or alternatively, call us on (08) 9200 3450.
If you are unsure of what vein condition you may have, assess your legs with our online tool.
If you are looking for cosmetic spider vein treatment only, please click here.