Perth's Leading Specialist in the Treatment of Varicose Veins
Dr Luke Matar | MBBS, FRANZCR, FACP
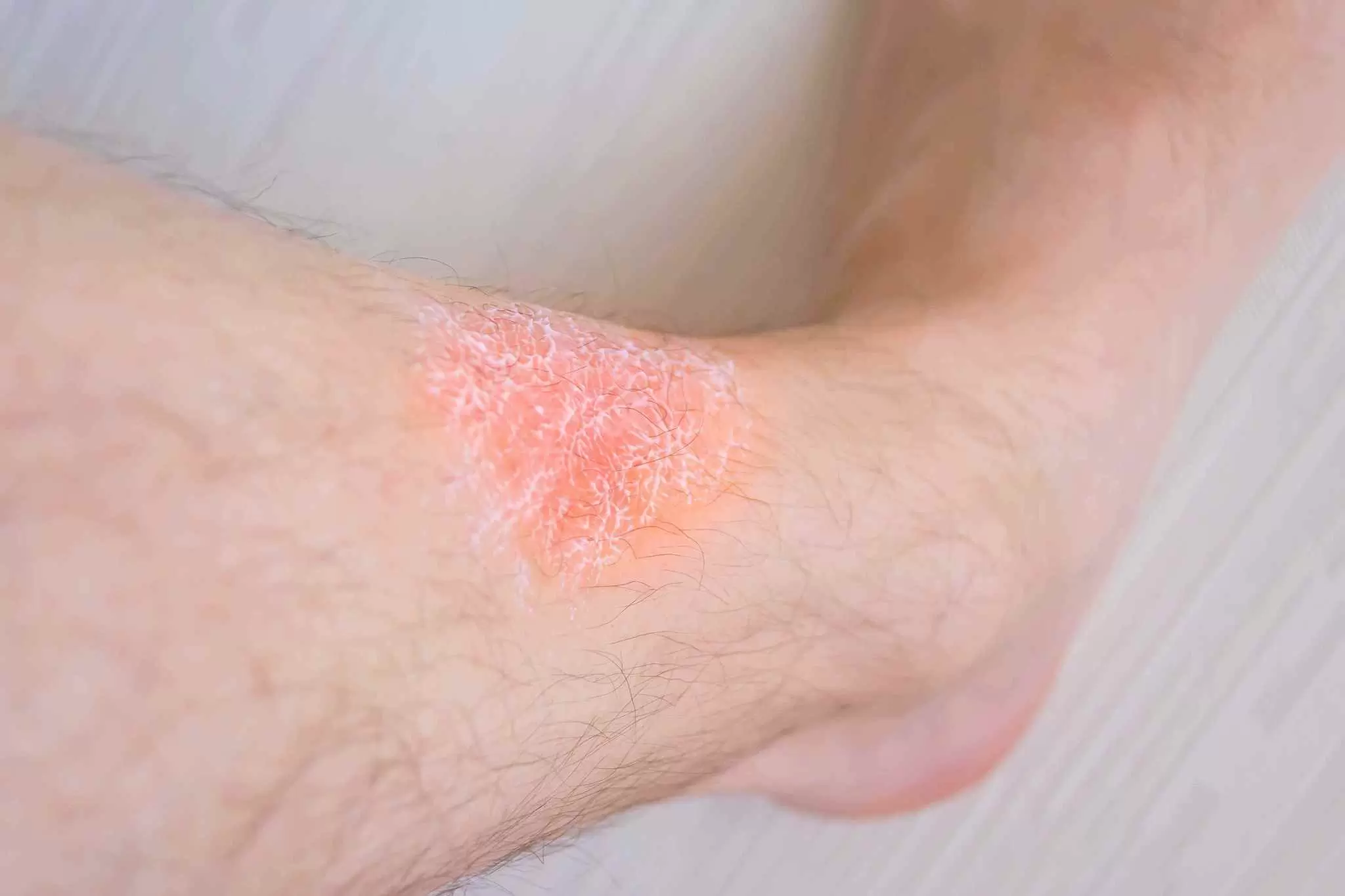
What is Stasis Dermatitis?
Stasis dermatitis, also known as venous eczema, varicose eczema or gravitational dermatitis, is an inflammatory condition of the skin seen in association with venous insufficiency also called venous reflux.
Venous eczema is more common in people with varicose veins, but not all patients with venous reflux and venous eczema will have visible varicose veins, as the varicose veins may be “hidden”. Without the correct varicose vein treatments, venous eczema may lead to chronic skin ulceration.
Stasis dermatitis is usually found around the ankles or lower legs and frequently misdiagnosed by general practitioners as cellulitis or simple eczema. Patients have typically struggled with this condition for many years with chronic relapsing.
Read MoreSymptoms of Stasis Dermatitis
If you experience the following symptoms around your ankles and lower legs (with or without varicose veins) it’s important to see a vein specialist.
- Itchy Skin
- Red & Swollen Skin
- Dry & Flaky Skin
- Scaly & Crusty Skin
What Causes Stasis Dermatitis?
Venous reflux occurs when the valves in the veins fail and blood travels toward the feet instead of the heart. This increases the pressure in the veins, which can cause fluid to leak into the surrounding tissues. It is thought that venous eczema may develop as a result of the immune system reacting to this fluid.
How To Treat Stasis Dermatitis
The first step in stasis dermatitis treatment is to book a consultation for a Doppler Ultrasound study. Once a diagnosis of venous reflux is confirmed, venous eczema can be cured by treating the underlying venous reflux.
There is no need to go on suffering when vein treatment could be a solution. We want to help you get an accurate diagnosis and effective treatment plan to address this often misdiagnosed medical condition.
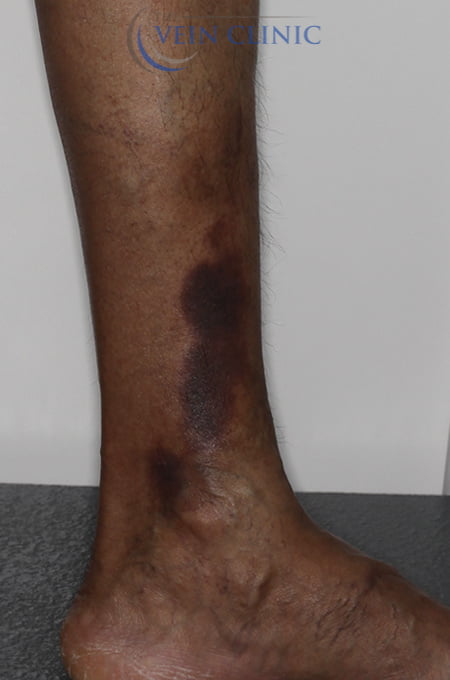
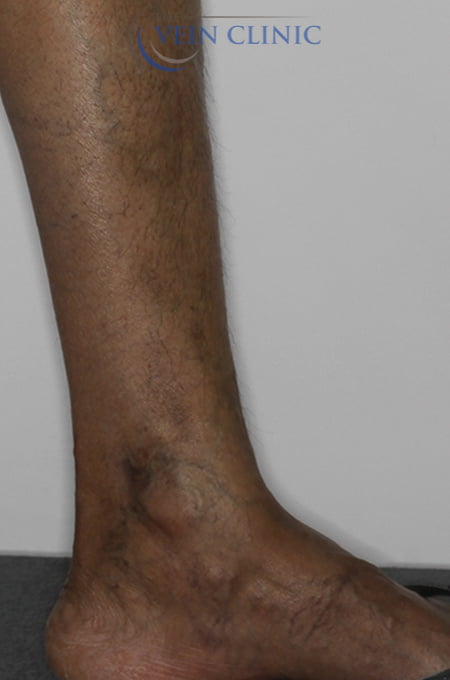
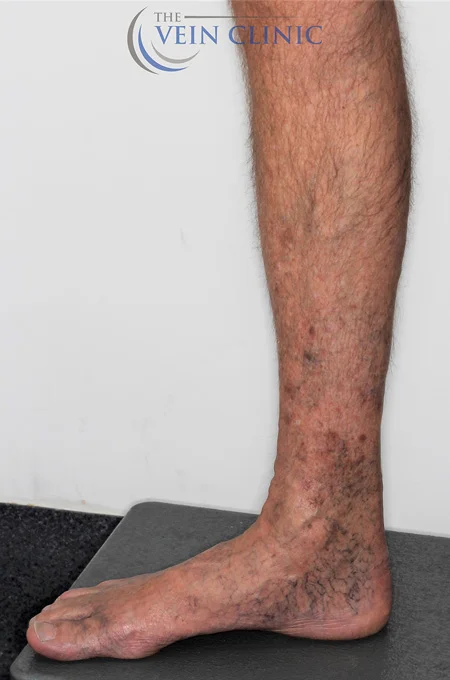
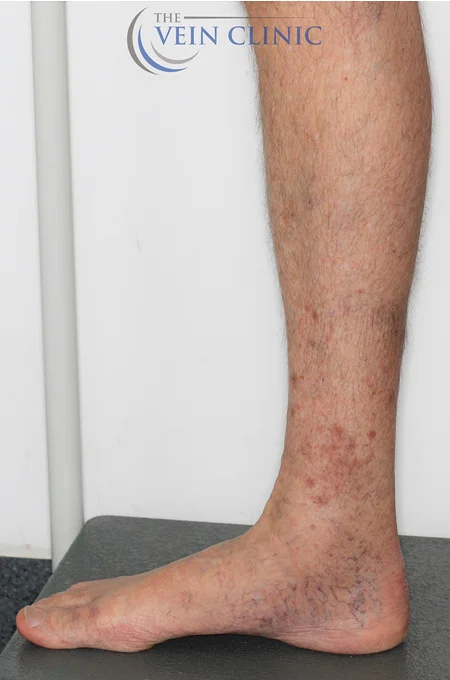
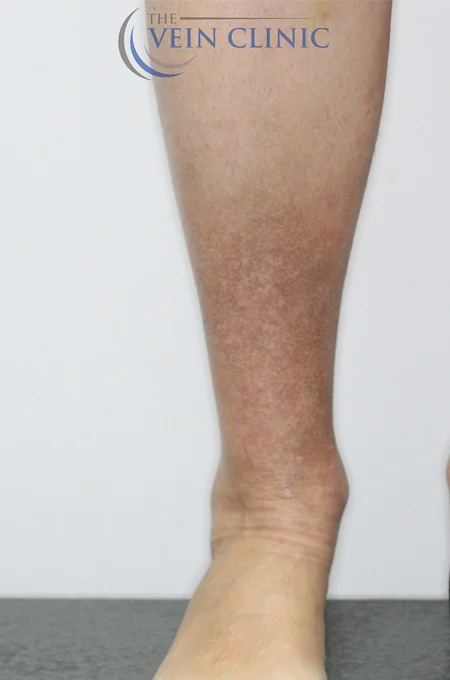
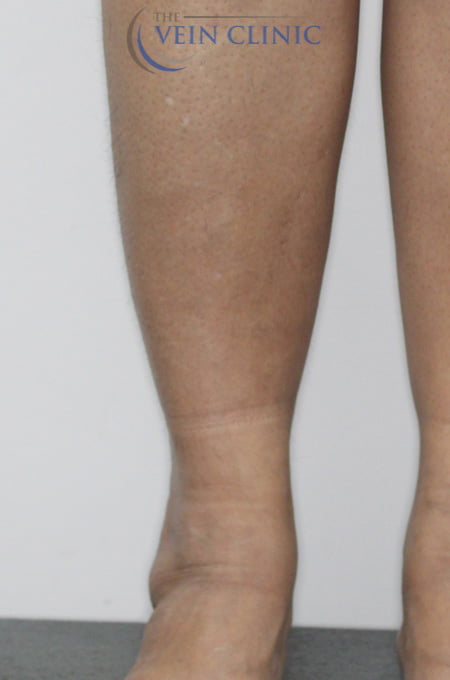
Stasis Dermatitis Treatment Before & Afters
Treatment Method
Bilateral Endovenous Laser Ablation & Ultrasound-guided Foam Sclerotherapy of the small saphenous vein, plus Ultrasound-guided Ambulatory Phlebectomy
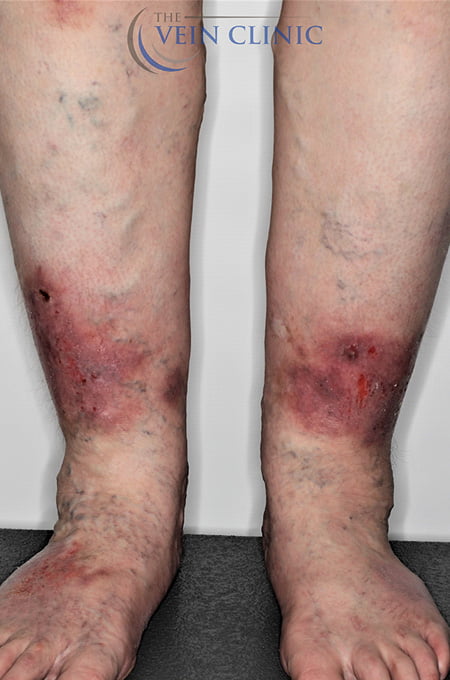
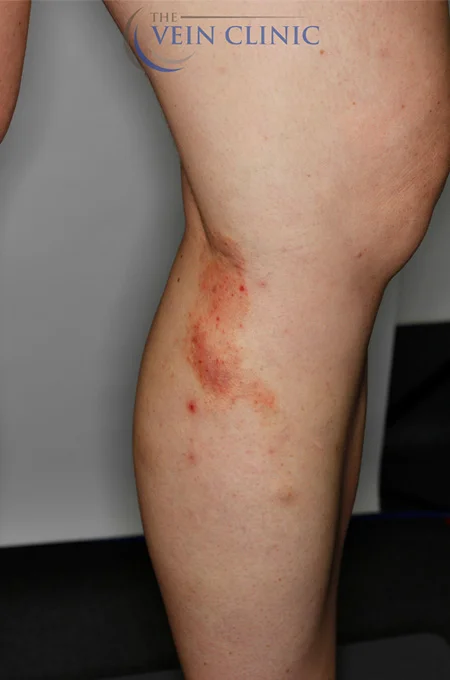
Read MoreTreatment Method
Endovenous Laser Ablation (right leg) and Ultrasound-guided Foam Phlebectomy
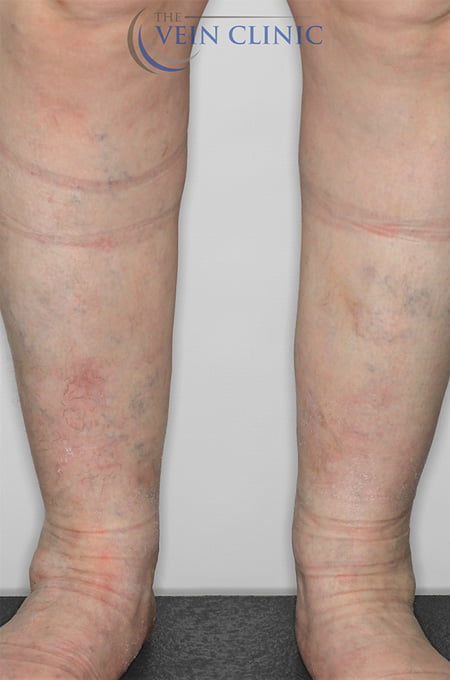
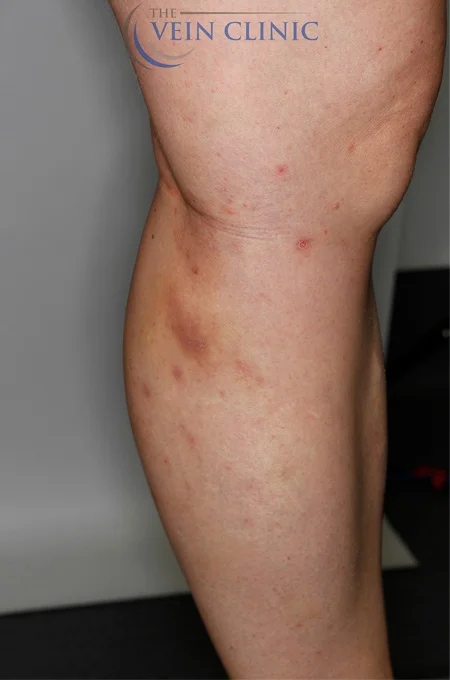
Read MoreTreatment Method
Endovenous Laser Ablation (right leg) & Ultrasound-guided Foam Sclerotherapy
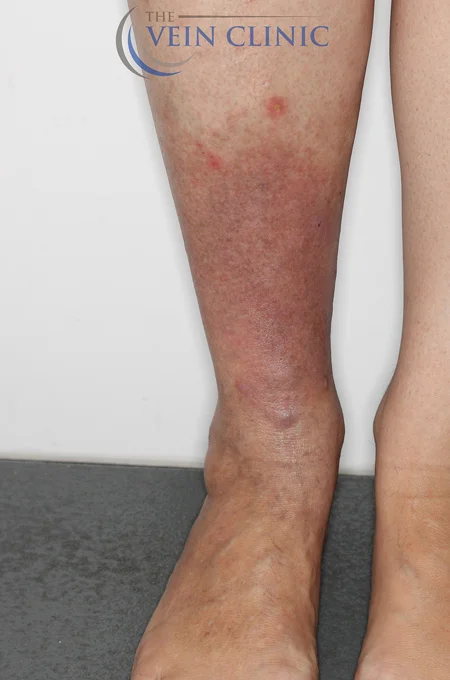
Read MoreTreatment Method
Endovenous Laser Ablation (right leg) & Ultrasound-guided Foam Sclerotherapy
Read MoreDiscover Our Advanced Treatments For Stasis Dermatitis
Non-Invasive, Non-Surgical Solutions
Based on your assessment in your consultation, Dr Matar will make recommendations about the most suitable treatment options.
At The Vein Clinic, we offer minimally invasive, non-surgical treatment options for varicose veins. They do not require a stay at the hospital and are performed at our state-of-the-art clinic in Subiaco. And because they are minimally invasive, you can return to your everyday life soon after your procedure.
Our Approach to Treatment
Stage 1
Treatment of large malfunctioning veins (trunk)

Endovenous Laser Treatment (EVLA) to great, small, and/or anterior accessory saphenous veins. 60 minutes
Stage 2
Treatment of large varicose veins (branches)

Phlebectomy removal of larger bulging varicose veins 90-120 minutescombined with

Ultrasound-Guided Foam Sclerotherapy (UGFS) on smaller veins. 30 minutes
Stage 2
Treatment of small varicose veins (branches) if required

Extra sessions of UGFS to close smaller veins if identified as required at post-treatment follow-up scan 30 minutes
You may not require this stage.
Stage 3
Optional treatment surface veins (leaves)

Usually done by Microsclerotherapy 30 minutes
Most patients require multiple treatment sessions to remove spider veins.
Stage 4

Follow up and maintenance to ensure best results
Experiencing Other Symptoms?
The below symptoms can also indicate underlying vein problems. If you are experiencing any of these combined with venous eczema let us know in your consultation.
Frequently Asked Questions
What is Venous Eczema
Venous Eczema, also called gravitational dermatitis, stasis dermatitis, and venous stasis dermatitis, happens when there is venous insufficiency or poor circulation in the lower legs. If left untreated, the skin can break down to form ulcers.
Who gets Venous Eczema and why?
Venous Eczema or stasis dermatitis often affects people with poor circulation or underlying venous insufficiency. You are most likely to develop this type of eczema if you have high blood pressure or varicose veins, or have had a deep vein thrombosis, phlebitis or cellulitis in the past. Other contributing factors include being overweight, immobility and swelling.
What are symptoms of Venous Eczema?
Venous Eczema can affect the feet or lower legs on one or both sides. Besides ankle swelling, early signs include orange-brown speckles of discoloration sometimes called cayenne pepper spots. These spots develop when pressure and swelling cause capillaries, the smallest blood vessels, to burst.
Other symptoms of stasis dermatitis include:
- redness in lighter skin tones that may appear brown, purple, gray or ashen in darker skin tones
- itching
- scaling
- dryness
Is stasis dermatitis painful?
Stasis dermatitis is often accompanied with swelling and redness of the skin. The area can be dry with scaling of the skin causing itchiness. It may be very painful but there may be no pain. Itchiness is also variable from mild to severe. Over time this can aggravate the skin and develop into a venous ulcer
What causes a venous ulcer?
Skin affected by varicose eczema is thin and unhealthy and can easily break down – as soon as this happens, the area should be treated to help the skin heal quickly. If left untreated, the small hole can deepen and widen, and the resulting wound is called a ‘varicose ulcer’ (also known as a ‘varicose ulcer’ or ‘stasis ulcer’). These ulcers are typically found just above the inside of the ankle. They often ooze and can attract bacteria, both of which can aggravate the surrounding skin, making the eczema even worse. Sometimes events can occur the other way round – varicose eczema can develop for the first time around an existing ulcer or wound on the lower leg, but treatment remains the same.
How to get rid Venous Eczema (stasis dermatitis)?
Treatment for stasis dermatitis includes identifying and treating its root cause as well as controlling its various symptoms. Physicians typically diagnose stasis dermatitis by examining the skin but may also run tests to check blood flow and to help identify the root causes of poor circulation.
Treatment can include:
- compression stockings to reduce swelling
- elevating legs above the heart every two hours to reduce swelling
- avoiding foods high in salt
- supplemental vitamin C and rutin, a plant pigment and antioxidant, to help keep blood vessels flexible and healthy
- for red or darker-colored, itchy skin, dermatologists may prescribe a topical corticosteroid to calm inflammation
- topical or oral antibiotic if skin is infected
How can I reduce the risk of developing varicose eczema?
There are a number of steps you can take to reduce the risk of developing varicose eczema. One key step is to improve the blood circulation in the legs; for example, by walking more, if possible, and elevating the legs when seated.
If you have varicose veins, or have had phlebitis or a deep vein thrombosis, you will need to give extra care and attention to your legs for the rest of your life, since varicose eczema can occur years later. Try to lose weight, if necessary. If you need help with weight loss, talk to your practice nurse or consider joining a local weight-loss group.
Varicose veins can be treated, consult your doctor if you think you have them. Veins near the surface of the leg are not essential and removal by laser under local anaesthetic (endothermal venous laser ablation) will eradicate them. Sometimes a special injection (sclerotherapy) into the veins can help. The longer prominent varicose veins are left, the less successful surgical treatment can be – so don’t ignore the problem.
Will I always have varicose eczema?
This type of eczema can be an ongoing problem. The condition can become worse and then settle down, but if you have a good skin care routine, and are taking steps to support the blood circulation in the legs; together, these actions will help prevent flare-ups.
Don’t be too worried if varicose eczema appears – extra care and attention to the area can often clear the problem and prevent the skin breaking down. However, you may be left with some discolouration of the skin as part of the post-inflammatory process.
Preventative measures are very important and should be continued long-term – you will find that once you get into a routine, they will soon become a way of life!
What if topical treatment doesn't work?
If your condition does not seem to be responding to topical treatment, your doctor may consider patch testing to check if you have developed contact dermatitis. This is usually done by a skin specialist (dermatologist).
You may also need to be referred to a doctor who specialises in veins (a Phlebologist). A deeper assessment of your veins by a Phlebologist will help identify if:
- Your varicose eczema has underlying varicose veins or venous insufficiency that needs to be treated.
- You have a leg ulcer which is not responding to medical treatment.
References:
Read More on Our Blog

5 Ways to Prepare for Your Vein Procedures
1. Get to know and love your stockings! We strongly recommend you buy your compression stockings well ahead of your […]
Read More
Don’t Be Fooled By Winter!
Cold weather constricts the veins and can make you feel “less symptomatic” – ie. the bothersome ache, pain, itch, heaviness, or tiredness in your legs could be less of an issue, or perhaps go away entirely.
Read More
Do I Need Varicose Vein Treatment?
Suffering from varicose veins? For too long patients have been told that treatment for varicose veins is “cosmetic only” and […]
Read MoreGet In Touch
Please send us an email and we’ll be in contact very soon or alternatively, call us on (08) 9200 3450.
If you are unsure of what vein condition you may have, assess your legs with our online tool.
If you are looking for cosmetic spider vein treatment only, please click here.