Perth's Leading Specialist in the Treatment of Varicose Veins
Dr Luke Matar | MBBS, FRANZCR, FACP
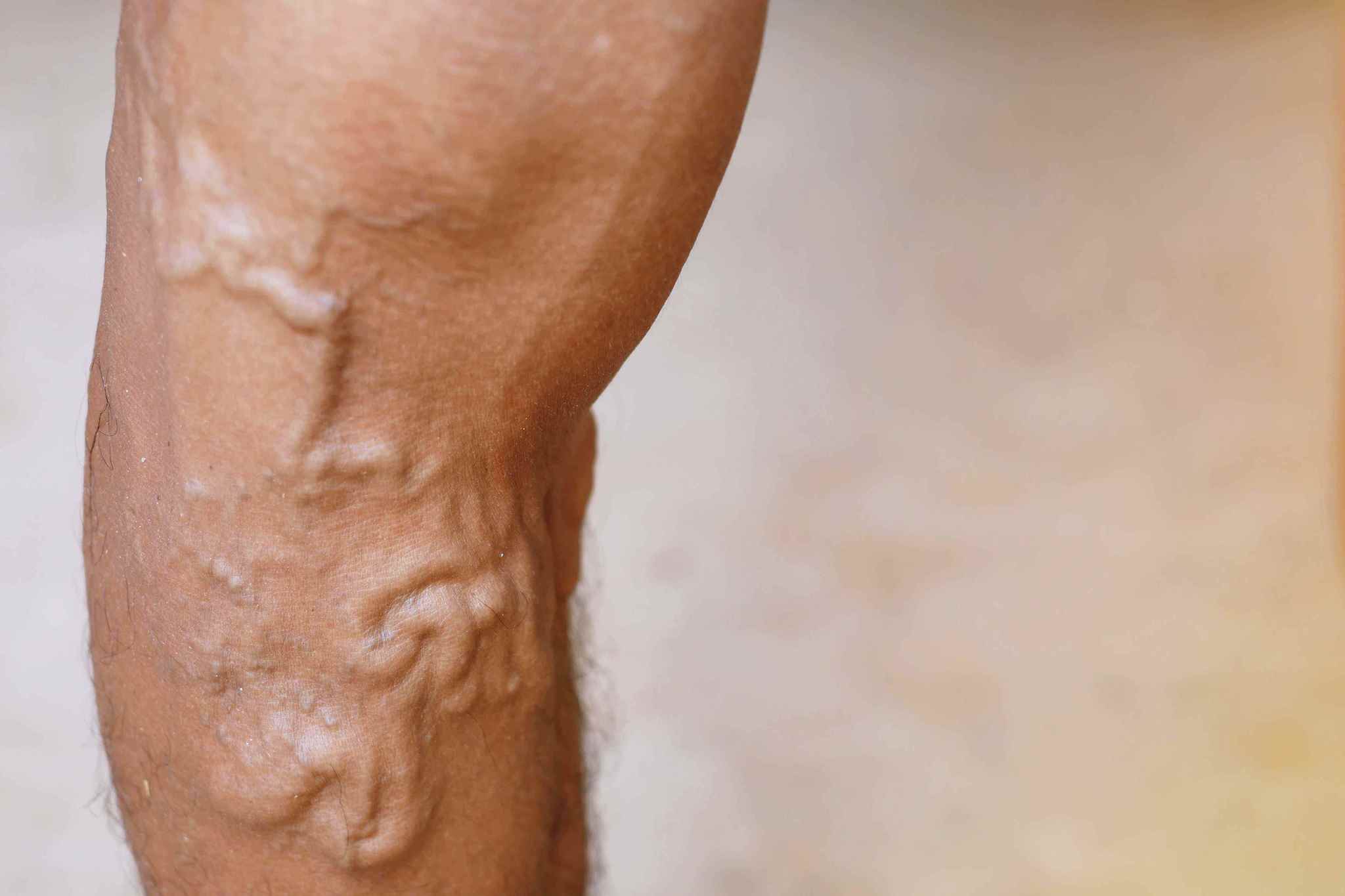
What Is Vein Stripping?
Vein stripping, also known as vein surgery, is an old-fashioned and harsh method of removing problem veins. Up until the 1980s, there was little option for treating varicose veins other than surgical vein stripping.
The treatment technique required hospital admission, where you would go under general anaesthetic and a large incision was made in the groin to allow for the saphenous vein to be identified and tied off. A wire stripper was placed down the saphenous vein initially to the level of the ankle and in more recent years to the level of the knee to minimise nerve injury with this surgery. The wire stripper would be pulled out through the lower incision stripping the vein from the level of the groin and ripping off all the side branches as it was removed.
At the Vein Clinic, we do not perform surgical vein stripping. Instead, we offer innovative and minimally invasive vein treatments.
Why We Don’t Perform Vein Stripping
There are many complications when it comes to varicose vein stripping. Vein stripping is a painful procedure that causes significant bruising and pain and requires patients to take up to two weeks off work. There’s also a high risk of developing deep vein thrombosis (DVT).
- Hospital Admission
- General Anaesthetic
- Significant Bruising
- Painful Recovery
- High Recurrence Rate
- DVT Risk
To make varicose vein stripping surgery even worse, there is a 50% recurrence rate at 5 years. Read our article Facts About Vein Stripping for more information.
This treatment type can drastically affect your everyday life and with the new, minimally invasive and highly advanced varicose vein treatment options now on the market, there is really no need to go down this path of vein removal.
The latest, innovative treatment options do not require hospitalisation, and you can often return to your normal activities immediately after your treatment. With improved recurrence rates, you will also be able to enjoy healthy, beautiful legs for longer.
Numerous international experts around the world agree that surgical vein stripping is no longer regarded as “best practice” for the treatment of varicose veins and venous insufficiency.
Organisations such as the Australian and American Colleges of Phlebology, American Venous Forum, and the International Union of Phlebology, now recommend more modern techniques such as endovenous laser ablation.
The National Institute for Health and Care Excellence (NICE) in the United Kingdom, included this in their 2013 Guidelines:
“Exercising, losing weight, avoiding tight clothes, elevating your legs, and avoiding long periods of standing can lessen pain and may help slow the progression of varicose veins from getting worse but will do nothing to get rid of varicose veins once established.
In some instances where the veins are very superficial and very extensive, surgery may be a reasonable option. It is recommended that before you commit to having surgical treatment of your veins you seek a second opinion from a vein specialist experienced in non-surgical treatments such as endovenous laser and ultrasound-guided sclerotherapy.”
Vein Stripping Alternatives
The Vein Clinic performs a range of the most technically advanced non-surgical options. We employ a variety of methods to minimise discomfort and downtime but more importantly to maximise effectiveness and long-term results whilst limiting disruption of your everyday life and activities.
Vein Stripping Vs Ambulatory Phlebectomy
These are two very different procedures.
Traditional vein stripping is an invasive procedure performed under general anaesthesia in hospital. In this procedure, the surgeon makes two incisions, one at the top of the affected vein in the groin and one in your calf or ankle. A wire stripper is then advanced through the vein, tied to the saphenous vein and pulled out, bringing the entire vein with it and ripping off the attached branch vessels, causing extensive bruising. After vein stripping, recovery is often prolonged and uncomfortable with patients generally requiring 1-2 weeks off work. | Ambulatory phlebectomy is a minimally invasive procedure performed under local anaesthesia as an outpatient at The Vein Clinic. In this procedure, larger bulging surface veins are physically removed through small incisions placed directly over the target veins. A small hook is placed through the incision to capture the vein and it is then gently removed through the incision. A surprisingly large amount of abnormal veins can be removed through incisions generally between 1-3mm in size. Dr Matar has pioneered the technique of performing phlebectomy under ultrasound guidance, improving the accuracy of incision placement and therefore the patient recovery. After phlebectomy, recovery is rapid and usually associated with minimal discomfort. Patients may return to office-based work the following day. |
Our Approach to Vein Treatment
Stage 1
Treatment of large malfunctioning veins (trunk)

Endovenous Laser Treatment (EVLA) to great, small, and/or anterior accessory saphenous veins. 60 minutes
Stage 2
Treatment of large varicose veins (branches)

Phlebectomy removal of larger bulging varicose veins 90-120 minutescombined with

Ultrasound-Guided Foam Sclerotherapy (UGFS) on smaller veins. 30 minutes
Stage 2
Treatment of small varicose veins (branches) if required

Extra sessions of UGFS to close smaller veins if identified as required at post-treatment follow-up scan 30 minutes
You may not require this stage.
Stage 3
Optional treatment surface veins (leaves)

Usually done by Microsclerotherapy 30 minutes
Most patients require multiple treatment sessions to remove spider veins.
Frequently Asked Questions
Why do I have varicose veins?
Most varicose vein issues are hereditary. If you have one parent with varicose veins your risk of having them is around 65%. If both parents are affected the risk rises to approximately 90%. Another main risk factor for women is pregnancy, with the risk increasing with each additional pregnancy. Standing occupations such as hairdressers, nurses, and chefs also have a high risk of varicose veins as gravity puts pressure on the veins and weakens them.
How do I prevent varicose veins?
Once varicose veins are present, they will not resolve of their own accord. Measures to reduce the rate of progression include maintaining a normal healthy weight and going for regular walks of 20-30 minutes per day. Reducing the length of time spent on the feet in a stationary position may help and alternating between standing and sitting positions during the day will also reduce the pressure on the veins.
What will happen if I don’t treat these veins?
Generally, without treatment, varicose veins will get progressively worse over time. Symptoms may occur such as heaviness, ache, pain, and tiredness in the legs towards the end of the day. Further progression may result in leg swelling, itch, skin discolouration, and eventual skin ulceration. Blood clots related to superficial venous thrombosis may also occur in severe cases and can lead to the more serious condition of Deep Vein Thrombosis.
What treatment options exist?
Outdated, old-fashioned options such as surgical stripping are rapidly becoming obsolete due to poor long-term success, with recurrence rates of up to 50%. Modern treatment options include endovenous laser ablation, sclerotherapy injections, and ultrasound-guided ambulatory phlebectomy. In many cases a combination of different treatments will give the best long-term results.
Will the veins come back after treatment?
Many people are concerned that the treatment will be of limited value because the veins will just come back. This was certainly the case in the days of surgical stripping with a 50% recurrence rate at 5 years; however, using the latest minimally invasive techniques, we can reduce the risk of recurrent varicose veins to the baseline risk of approximately 3% per year.
What is the downtime following treatment?
This depends on the type of procedure performed and the severity of the veins being treated. Modern treatment with laser can involve no time off work and approximately two weeks off heavy gym work and four weeks off international travel.
Get In Touch
Please send us an email and we’ll be in contact very soon or alternatively, call us on (08) 9200 3450.
If you are unsure of what vein condition you may have, assess your legs with our online tool.
If you are looking for cosmetic spider vein treatment only, please click here.